Will Medicaid Cover Braces for Kids and Adults? Answered!

Will Medicaid Cover Braces? Everything You Need to Know
Dental care from orthodontists, especially when it includes braces, can be one of the largest medical bills a family faces. This is particularly true for teens whose parents are trying to straighten teeth on a limited budget. If a family is enrolled in Medicaid, the main question they are asking is usually simple:
“Will Medicaid help pay for braces?”
Medicaid is a public assistance program aimed at offering health care to people with low or moderately low income, but one size does not fit all; the details of what it pays for can differ widely from one state to the next. This guide walks you step by step through the basics of Medicaid coverage for orthodontic work, the medical justifications generally required to get the program to agree to pay the cost, and the practical to-do list you should execute to find out whether and how your own family can tap into Medicaid help for orthodontic expenses.
What Is Medicaid?
The following explanation of braces coverage requires prior knowledge about Medicaid. Medicaid operates as a joint federal-state program which provides low-income people with access to fundamental healthcare services including medical and dental and mental health care. The Medicaid program operates through state administration with flexible guidelines that result in different coverage options based on your location. The Medicaid program provides coverage to people who fulfill particular eligibility criteria which typically include income level and age and family size requirements.
Medicaid Dental Coverage
Medicaid not only funds hospitals and primary-care visits, it also pays for dental services. For youth under 21, coverage isn’t optional: every state must include it under the EPSDT program, designed to catch health needs early. For grown-ups the rules shift, and coverage is patchwork. Some states cap care to the basics—extractions and pain relief—while others stretch the benefit to include preventive cleanings, crowns, and even dentures. The range is detailed, so reviewing your state’s specific guidelines is always wise.
Does Medicaid Cover Braces for Children?

When kids are enrolled in Medicaid, the program often offers wider-ranging support for braces. Since the law requires that all dental services for kids go through the EPSDT—Early and Periodic Screening, Diagnosis, and Treatment—most orthodontic care is covered so long as it’s deemed medically necessary. Still, the program sets some specific criteria that a dentist must show are met before it pays for the braces.
Medically Necessary Treatment
Medicaid pays for orthodontic treatment among kids only when the braces are considered medically essential. Work meant only for improving looks doesn’t get any benefits. Help is usually allowed when severe dental problems are present—problems that might interfere with good nutrition, talking clearly, or maintaining healthy gums and teeth.
Some conditions that may qualify a child for braces under Medicaid include:
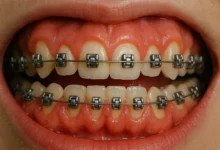
Severe malocclusion: A condition where the teeth are misaligned in a way that affects the bite, chewing, or speaking.
Crossbite: When the upper teeth do not come down slightly in front of the lower teeth.
Overbite: When the upper teeth excessively overlap the lower teeth.
Underbite: When the lower teeth protrude further than the upper teeth.
Open bite: When the teeth do not meet when the mouth is closed.
The orthodontist evaluates dental conditions of children to establish medical necessity for braces. The Medicaid program will cover necessary treatment expenses but you need to pay co-pays and other out-of-pocket costs according to your state’s program requirements.
State-Specific Medicaid Coverage for Braces
The majority of states expanded orthodontic coverage beyond medical necessity cases yet their specific requirements differ substantially. Several states determine eligibility through specific criteria which include severe malocclusion and documented airway obstruction. The coverage period for orthodontic treatment ends when children reach a specific age under some plans while others require families to submit recent cephalometric x-rays and peer-reviewed assessments demonstrating health benefits from treatment. The following summary presents a comparison of Medicaid orthodontic benefits between various jurisdictions:
Medicaid Coverage for Braces in California
In California, Medicaid—called Medi-Cal here—will pay for kids to get braces as long as a dentist certifies the work is medically justified. Coverage is usually granted when a child’s bite is severely misaligned, for instance, if the upper teeth set too far forward or if the top and bottom teeth don’t line up properly.
The braces benefit extends to beneficiaries up to age 21, following the overall Medi-Cal age limit for routine dental services. For adults on Medicaid, the braces benefit is almost never available; any exceptions have to be clearly tied to a recovery from injury or to dental complications directly caused by a documented medical diagnosis.
Medicaid Coverage for Braces in New York
In New York, Medicaid pays for braces for kids younger than 21 when they’re necessary for health—not just for appearance. Coverage kicks in if misaligned teeth cause real problems, like pain when chewing, trouble making sounds, or other serious everyday challenges. Adults generally won’t find orthodontic work in Medicaid plans, unless a clear medical reason supports it, like a jaw injury or a procedure needed to manage another health issue.
Medicaid Coverage for Braces in Florida
Florida Medicaid helps kids younger than 21 keep their smiles healthy by providing orthodontic coverage when dental problems are serious enough to impact their oral health. Coverage for braces is available for children with issues like malocclusion, crossbites, and other severe bite problems. Adults, on the other hand, won’t see orthodontic treatment covered unless there’s clear medical need as supported by documentation.
Does Medicaid Cover Braces for Adults?

Medicaid has tighter rules on braces for adults than for minors. Still, grown-up Medicaid recipients can squeeze in a few mouth-visit perks. Regular dental care is there for the taking, yet the real prize—braces—will likely cost the patient a few bucks unless a doctor files a solid, medical-necessity letter. Proof of an underlying health condition, like jaw issues that affect chewing or an uneven bite that leads to gum breakdown, is the ticket that gets the claim past the gatekeepers.
Medical Necessity for Adult Braces
In certain cases, adults may qualify for braces if they have a condition that makes orthodontic treatment necessary for their overall health. For example:
Teeth that cannot be properly cleaned: The Medicaid program will cover braces when misaligned teeth create oral hygiene challenges that result in higher risks of gum disease or tooth decay.
Jaw or bite problems: Braces may be considered medically necessary for adults who experience jaw or bite problems that lead to pain or eating and speaking difficulties.
Trauma or injury: Orthodontic treatment following a traumatic injury that affects tooth alignment may be covered under Medicaid in certain situations.
State Variations
The availability of adult Medicaid orthodontic benefits depends on the specific state where you live. The availability of adult orthodontic benefits through Medicaid depends on state policies because some states provide coverage for medically necessary orthodontics but others do not offer any benefits for braces. You should verify the available benefits through your state Medicaid program.
How to Qualify for Medicaid Coverage of Braces
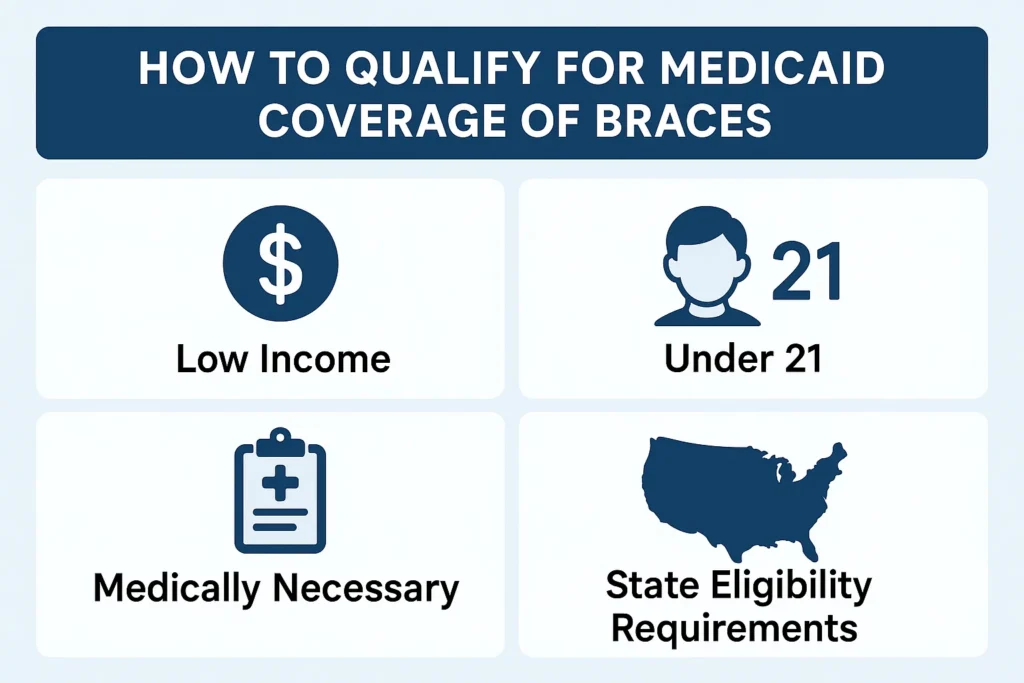
If you believe that you or your child may qualify for Medicaid coverage of braces, there are several steps you can take to determine eligibility and start the process:
Step 1: Confirm Medicaid Eligibility
Check first if you or your child qualifies for Medicaid before starting any braces or alignment plan. The answer hinges on household income, child’s age, family size, and a few additional criteria. The simplest way to apply is to visit your state’s health department or the local social services office. Typically, Medicaid decides on eligibility every year, meaning you’ll have to update or renew the coverage application within that same annual period.
Step 2: Visit an Orthodontist
After you get your Medicaid card, the next thing to do is schedule an evaluation with an orthodontist. The doctor will look at the teeth to see whether your or your child’s bite or alignment needs correcting. If the braces are judged medically necessary, the orthodontist will fill out the paperwork. That paperwork is sent to Medicaid to get the treatment approved.
Step 3: Obtain Authorization from Medicaid
Once your orthodontist hands you the required paperwork, the next step is to send a Medicaid approval request. In that request, you’ll outline the reasons braces are medically necessary, citing any health issues or everyday problems that the misalignment is causing. Medicaid will look over the whole file, then decide whether the treatment will be paid for.
Step 4: Understand State-Specific Limitations
Remember, Medicaid coverage for braces varies by state, so knowing your state’s guidelines is crucial. To find out what’s covered, reach out to your local Medicaid office, or ask the orthodontist for help—they’ll know the most up-to-date rules.
Alternatives When Medicaid Doesn’t Cover Braces

If Medicaid does not cover braces or only offers limited coverage, there are alternative options you can explore:
1. Dental Discount Plans
In some states, discount plans that focus strictly on dental care deliver solid savings on orthodontic work, particularly when it comes to braces. These arrangements trim the amount families must pay at the time the treatment is delivered, making it easier to budget for the care a child needs.
2. Payment Plans or Financing Options
Orthodontists provide flexible payment plans to their patients for covering braces expenses. The payment plans enable patients to distribute their braces expenses across multiple time periods thus decreasing the financial impact of braces treatment.
3. State-Specific Programs
Some states have particular programs which assist low-income families with orthodontic care expenses. These programs are not Medicaid programs but they do offer financial assistance for braces to those who qualify.
4. Private Insurance
The Medicaid program does not provide coverage for braces but private dental insurance plans may offer orthodontic benefits to their subscribers. Private insurance plans provide coverage for braces expenses either fully or partially for both children and adults.
Conclusion: Will Medicaid Cover Braces?
To wrap up, braces for kids will be paid for by Medicaid when the care is shown to be medically essential, but the rules about what that means vary from state to state. For adults, coverage is rare unless the treatment is tied to a documented health problem. Make sure to reach out to the Medicaid office in your state so you can see exactly what your plan wraps around—and whether you can even get braces treatment in the first place.
Once you know what the agency covers, you can review the requirements that you have to meet and weigh possible pay-the-full-price or discount options. With all that in hand, you can decide confidently how to go ahead with braces.
Average Cost for Braces Per Month in 2025: What You Really Pay